Robotic Assistance in Interventional Radiology
- Dr Tarangini V
- May 2, 2022
- 4 min read
Updated: May 3, 2022
What is Interventional radiology?
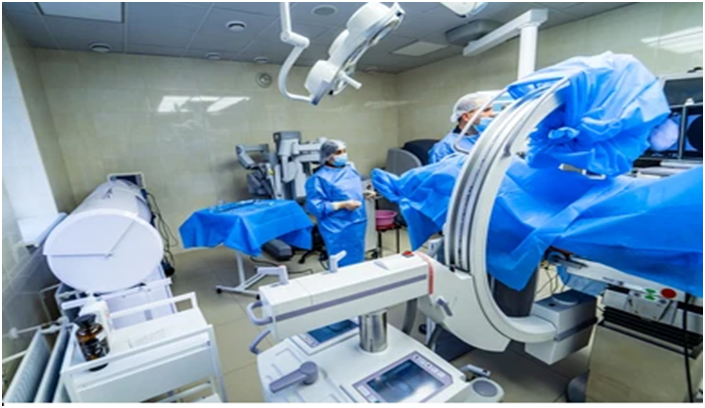
Interventional radiology is a clinical sub-uniqueness of radiology making use of minimally-invasive image-guided strategies to diagnose and deal with illnesses in almost each organ system.
Image credit: Shutterstock
Interventional radiology has grown dramatically since its inception in 1953. Robotic support in medicine was a revolution. It began with a stereotactic brain tumor biopsy in 1988 based on computer tomographic images. In 1988, it gradually achieved multiple surgical applications, including robotic assistance in cardiac surgery for aneurysms and repair of large atrial septal defects by endoscopic manipulation.
The use of robots has naturally expanded to interventional radiology for percutaneous and intravascular procedures. First-generation robots helped point the needle at two degrees of freedom. Second, the robot was given up to six degrees of freedom and extended intervention options. Developed at the Johns Hopkins Medical Institution's U Robotics Laboratory, the AcuBot robot provided an accuracy of 2 mm. Its use was practical, safe, and rapid for biopsy or percutaneous resection of various organs. Guidance is primarily remote control (computer or joystick), so the operator and his team are not exposed to X-rays.
What are the machines used in Interventional Radiology?
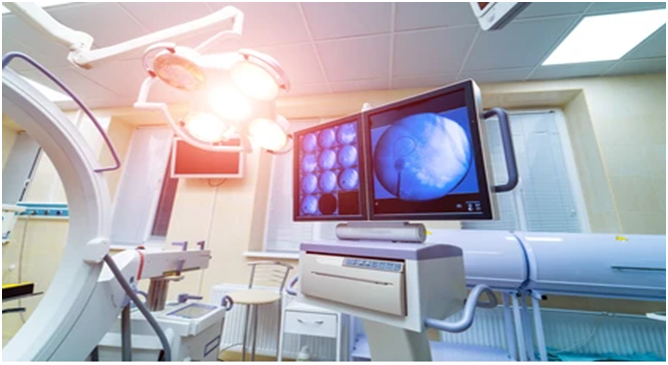
Interventional radiology (IR) consists of a wide variety of equipment that is essential for both diagnostic and therapeutic procedures. Common diagnostic imaging procedures used include fluoroscopy, ultrasound, computer tomography, and magnetic resonance imaging.
Why does Interventional Radiology need Robotics?
It is generally assumed that intervention specialists can use minimally invasive methods to reach cavities with pinpoint accuracy in almost any area of the body. So, why do you need a robot? There are advantages to implementing a robot.
First, learning to operate a robot to perform complex intervention procedures means that the radiologist can move away from the suite in which the procedure is being performed and therefore not be exposed to radiation.
Second, robotic equipment is designed with multiple degrees of freedom in navigation and is more dexterous than the average human being. This means that in patients with complex anatomy, navigating the intervention device is easier and therefore safer.
Third, modern robotic equipment works magnetically, making magnetic resonance imaging (MRI) guided procedures faster and more accurate. This is very exciting. MRI-guided interventions provide immediate, real-time feedback on treatment with functional parameters. One of the biggest challenges for penetrating surgical robots is the need for a stable power source combined with a wireless connection. It is being investigated how MR scanners can be used to maintain wireless power.

Image credits: Shutterstock
Robotic-assisted interventional radiology:
Robotic assistance in interventional radiology procedures is gaining traction rapidly. An emerging clinical practice is closely following the growth of the robotic interventional healthcare industry. This industry is concentrated on revolutionizing how interventional procedures are performed.
Presently, robotic assistance can be combined with ultrasound, magnetic resonance imaging (MRI), computed tomography (CT), and fluoroscopy. The benefits of robotic assistance in interventional procedures with these modalities are clear: greater operator precision and control. This upgraded accuracy can lead to reduced procedural time, radiation exposure, recovery time, procedural complications and mortality. An extra advantage is remote operator use. Tele-operation can reduce radiation exposure to the operator and also provide remote patient access. The latter could be of use when operator assistance is needed.,
Researchers have focused on such areas as image-guided biopsies, ablations, and endovascular interventions. Robot biopsies and excisions are performed using a robotic device mounted on a tabletop or patient. Koethe et al. In a phantom model evaluating needle insertion for CT-guided biopsy and high-frequency ablation. Reduced needle tips to target errors on robot platforms and improved needle placement accuracy.
As with all healthcare innovations, quality control and assurance measures are needed. This includes guidelines for proper use, technical performance, and training of physicians and technicians. Through these behaviors and ongoing research and development, the future of interventional radiology is defined by the safe clinical use of robotic technology. During the 2016 Strategic Planning session, interventional lists and healthcare managers will need to embrace this exciting innovation for their ability to improve interventional radiology and patient care.
References
Koethe Y, Xu S, Velusamy G, Wood BJ, Venkatesan AM. Accuracy and efficacy of percutaneous biopsy and ablation using robotic assistance under computed tomography guidance: a phantom study. Eur Radiol. 2014; 24(3):723-730
Anzidei M, Argiro R, Porfiri A, Boni F, et al. Preliminary clinical experience with a dedicated interventional robotic system for CT-guided biopsies of lung lesions: a comparison with the conventional manual technique. Eur Radiol. 2015;25(5):1310-1316.
Stoianovici D, Kim C, Srimathveeravalli G, Sebrecht P, et al. MRI-Safe Robot for Endorectal Prostate Biopsy. IEEE ASME Trans Mechatron. 2013; 19(4):1289-1299
Bismuth J, Duran C, Stankovic M, Gersak B, Lumsden AB. A first-in-man study of the role of flexible robotics in overcoming navigation challenges in the iliofemoral arteries. J Vasc Surg. 2013;57(2Suppl):14S-9S
Rolls AE, Riga CV, Bicknell CD, Regan L, Cheshire NJ, Hamady MS, Robot-Assisted Uterine Artery Embolization: A First-in-Woman Safety Evaluation of the Magellan System. J Vasc Interv Radiol. 2014; 25(12):1841-1848
Lu WS, Xu WY, Pan F, Liu D, at al. Clinical application of a vascular interventional robot in cerebral angiography. Int J Med Robot. 2015; Mar 17 (Epub ahead of print).






Comments